Chilling Disparities Revealed: Emergency Care Quality for Patients with Substance Use and Mental Health Disorders
2025-03-31
Author: William
Background
Patients grappling with substance use disorders and mental health issues experience alarmingly high rates of morbidity and mortality, particularly when both conditions coexist—a phenomenon known as dual diagnosis. A groundbreaking study in Denmark has shed light on the stark realities of prehospital care (Emergency Medical Services, or EMS) and emergency treatment for time-sensitive medical issues among these vulnerable populations.
Methods
The researchers harnessed data from three extensive Danish registries spanning several years: the Danish Prehospital Registry (2016–2017), the Danish Stroke Registry (2010–2018), and the Danish Registry of Emergency Surgery (2008–2018). They scrutinized the quality of care using well-defined clinical metrics. Patients were categorized into four groups: those with mental illness, those with substance use disorders, those with dual diagnoses, and a reference group without these conditions.
Results
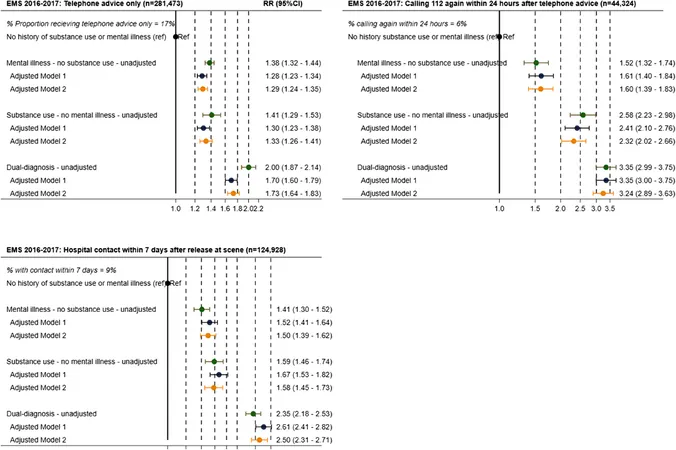
The study analyzed an astounding 492,388 EMS calls, 89,148 ischemic stroke admissions, and 3,223 surgeries for perforated ulcers. Alarmingly, mental illness, substance use disorders, and dual diagnoses were most notably present in the EMS cohort, affecting 10%, 9%, and 8% of calls, respectively.
Patients with these conditions were significantly more likely to experience repeat EMS calls and unplanned hospital visits shortly after being released at the scene. For instance, those with dual diagnoses had a staggering 3.24 times higher chance of calling EMS again within 24 hours. Additionally, stroke patients suffering from mental health issues or substance use were markedly less likely to receive life-saving reperfusion therapy.
Delays in emergency surgery for perforated ulcers also plagued these individuals, with mental health patients experiencing an average delay of 82 minutes compared to the reference group. Strikingly, within 90 days post-surgery, individuals with mental illness, substance use disorders, and dual diagnoses lost a median of 4, 6, and 7 days of life outside the hospital respectively.
Conclusions
The findings starkly illustrate the inequities in the quality of emergency care across various patient populations. Patients with mental health and substance use disorders face significant barriers, leading to suboptimal care and poorer health outcomes. While some aspects of care, like adherence to guideline-based stroke protocol, showed relative consistency, glaring disparities necessitate urgent reforms.
A Call to Action: Redressing Systemic Inequities
The study's results scream for comprehensive reforms in healthcare systems to provide integrated care solutions that merge mental health and substance use treatments effectively. The lack of coherent programs leaves many individuals relying heavily on emergency services for urgent needs, further highlighting the inadequacies preventing access to consistent, preventative care.
Future interventions should focus on reinforcing primary care and community support systems, particularly for high-risk populations, to diminish their dependence on emergency care. Emulating models like Assertive Community Treatment (ACT) and Patient-Centered Medical Homes (PCMH) could significantly enhance access, reduce reliance on emergency services, and ultimately promote better health outcomes.
The healthcare landscape must cultivate integrated strategies to address the unique vulnerabilities faced by those living with dual diagnoses. By confronting stigma head-on and ensuring timely, equitable care across all patient populations, health systems can begin to bridge the gap that has long existed within emergency medical services.
This study is a clarion call for healthcare providers, policymakers, and community leaders to unite in the fight against disparities, aiming to create an equitable healthcare system that serves all citizens effectively.
Final Thoughts
Do patients with dual diagnoses truly receive the care they need? The answer is overwhelmingly clear—if effective solutions are not implemented, countless lives will continue to be jeopardized. Are you ready to be part of a healthcare revolution that prioritizes the well-being of those who are often overlooked? The time for change is now.









 Brasil (PT)
Brasil (PT)
 Canada (EN)
Canada (EN)
 Chile (ES)
Chile (ES)
 Česko (CS)
Česko (CS)
 대한민국 (KO)
대한민국 (KO)
 España (ES)
España (ES)
 France (FR)
France (FR)
 Hong Kong (EN)
Hong Kong (EN)
 Italia (IT)
Italia (IT)
 日本 (JA)
日本 (JA)
 Magyarország (HU)
Magyarország (HU)
 Norge (NO)
Norge (NO)
 Polska (PL)
Polska (PL)
 Schweiz (DE)
Schweiz (DE)
 Singapore (EN)
Singapore (EN)
 Sverige (SV)
Sverige (SV)
 Suomi (FI)
Suomi (FI)
 Türkiye (TR)
Türkiye (TR)
 الإمارات العربية المتحدة (AR)
الإمارات العربية المتحدة (AR)